The shoulder is a ball and socket joint. Most of the shoulder movement occurs where the ball at the top of your arm bone(‘humeral head’) fits into the socket(‘glenoid fossa’), which is part of the shoulder blade (‘scapula’). The arm is normally held in the socket by the soft tissue which fits over the joint liked a sock. This is stabilized by fibrous tissue in the capsule, and by the muscles and tendons that rotate the arm, but there is still a large amount of freedom in the joint. The shoulder is an inherently unstable joint. This joint can move in almost all directions which allows us to throw a baseball, spike a volleyball, hang from a pull-up bar, and reach behind our backs to scratch an itch. This freedom of motion comes at the expense of overall stability.
Shoulder dislocations typically occur from sudden jarring motions while the shoulder is in a compromised position. The force required to do this can also tear or partially tear the muscles, ligaments and/or shoulder capsule surrounding the joint. An auto accident, fall off a bicycle, or collision while playing sports are common examples of situations that can cause dislocations. For those who are naturally hyper-flexible, it may take much less force to cause a dislocation.
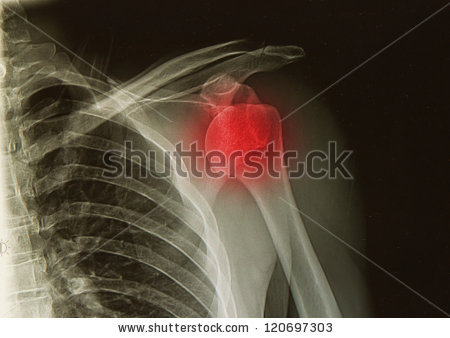 Shoulder dislocations most often occur “anteriorly,” meaning that the head of the humerus bone spills out of the joint in a forward direction. The above photo of a baseball pitcher is an example (albeit an extreme one) of a dislocation position.
Shoulder dislocations most often occur “anteriorly,” meaning that the head of the humerus bone spills out of the joint in a forward direction. The above photo of a baseball pitcher is an example (albeit an extreme one) of a dislocation position.
Shoulder Rehabilitation
Once the shoulder has been restored to its normal position in its socket, this is just the beginning of the rehabilitation process to work on strengthening the surrounding muscles once you are cleared by your doctor to begin exercise It is important for you to strengthen your shoulder fully and to be able to move it through a range of movements without experiencing pain. It is of vital importance that you do not place your arm in extreme positions during the early phases of rehab.
If you have dislocated your shoulder, it is a good idea to work on strengthening the surrounding muscles once you are cleared by your doctor to begin exercise. It is of vital importance that you do not place your arm in extreme positions during the early phases of rehab. Stick to “isometric exercises” at first. Isometrics involve placing resistance on the muscles of the shoulder while the shoulder itself is not moving.
The rehabilitation process can be split up into three phases.
Phase 1 :
This phase starts after the shoulder has been put back into its socket. The polysling we have given you will help to keep your shoulder comfortable. It should be worn for a maximum of two weeks, unless you have also broken your shoulder, when you have to wear it for up to six weeks.
Pain can be a problem particularly in the first 2-3 weeks. Your doctor may give you a prescription to help with pain relief, or you can control the pain with basic painkillers, such as paracetamol. Also, you may benefit from putting an ice pack (e.g. a bag of frozen peas in a damp towel) on the area for 10-15 minutes.
Your physical therapist will give you some gentle movements for the arm, out of the sling, to help reduce stiffness and relieve some of the pain. Your physical therapist will also highlight the importance of good upright posture with your shoulder muscle balance in the future.
It is important during this stage that you avoid positions that could cause re-dislocation. The most important position to avoid is holding your arm out at 900 degrees to your side with the palm facing upwards, especially if a force is being applied.
Phase 2 :
The main focus of this phase is to increase your range of movement further, increase your muscle strength, especially your rotator cuff, and to re-establish the muscle balance in your shoulder. Your progress will depend on the nature and severity of your injury.
The rotator cuff is a group of muscles that rotate the arm, and form a cuff or sleeve around the shoulder joint and capsule. These must work together to keep the shoulder still whilst moving the arm. The physical therapist will identify any weakness in these muscles and give you exercises to strengthen them. Please follow what the physical therapist has told you when doing the exercises.
The scapula is supported by two important muscles, the trapezius muscle and the serratus anterior muscle. These muscles must be strong to control the shoulder blade as the shoulder joint moves. The physical therapist will assess the muscle control of the scapula and give you an appropriate exercise program as necessary.
Phase 3 :
The aim of this phase is to make progress towards functional and sporting activities, by helping to regain the neuromuscular control of your shoulder. This is achieved by exercising the unstable shoulder in positions that challenge the shoulder muscles fully.
This also re-trains your proprioception, which is your body’s awareness of where a limb is in space. This works by messages relating to joint position awareness being sent to the brain via receptors in the shoulder. When these receptors detect a situation of potential tissue damage, the muscles are caused to contract by the brain. This then causes the joint to move, so decreasing the mechanical stress on the surrounding areas.
The physiotherapist will give you exercises that are as similar as possible to the movements you do during your sporting activities.
Exercises
- Use pain-killers and/or warm compress to reduce the pain before you exercise.
- It is normal for you to feel aching, discomfort or stretching when doing these exercises. However, if you experience intense and lasting pain (e.g. more than 30 minutes), it is an indication to change the exercise by doing it less forcefully, or less often. If this does not help then please discuss this with your physical therapist.
- Do short frequent sessions (e.g. 5-10 minutes, 4 times a day) rather than one long session.
- Gradually increase the number of repetitions that you do.
- Aim for the number of repetitions your PT advises (the numbers given here are rough guidelines).
- Get into the habit of doing them!
What If you re-dislocate your shoulder?
Most orthopedic surgeons will agree that if shoulder dislocations occur multiple times within the scope of a few years despite conservative management, surgery is in order. Dislocations will very often coincide with tearing of the “labrum” of the shoulder. The labrum is a cartilaginous ring that surrounds the socket and provides additional stability to the joint. Once the labrum is torn, there is even less stability in the shoulder and active motions are more likely to become chronically painful despite strengthening around the joint. The labrum can be surgically repaired and normal function restored, but it is indeed a long process that requires diligence and patience. Make sure that you have pursued a conservative approach that involves strength training prior to considering surgery if you have suffered a shoulder dislocation!
We can provide you physical therapy home service to guide you for the protocols.
References:
Oxford Radcliffe Hospital
PhysioDC http://www.physiodc.com/how-do-i-deal-with-a-shoulder-dislocation/
